Dose Dependency and
the Mechanism of Carcinogenesis
1. How much radiation exposure causes cancer?
There is no dose (“threshold”) below which exposure will not cause cancer. This means there is no safe radiation dose. Since the risk of radiation exposure is cumulative, risk is estimated by totaling the exposure doses.
The relationship between radiation dose and the incidence of cancer is shown in the figure below, where the incidence increases in proportion to dose. For example: if 10,000 people are exposed to 1 millisievert, 1 person will develop cancer, and if they are exposed to 10 millisieverts, 10 people will develop cancer. This is called the Linear No-Threshold (LNT) model, and the International Commission on Radiological Protection (ICRP) recommends that radiation protection should be based on this model.
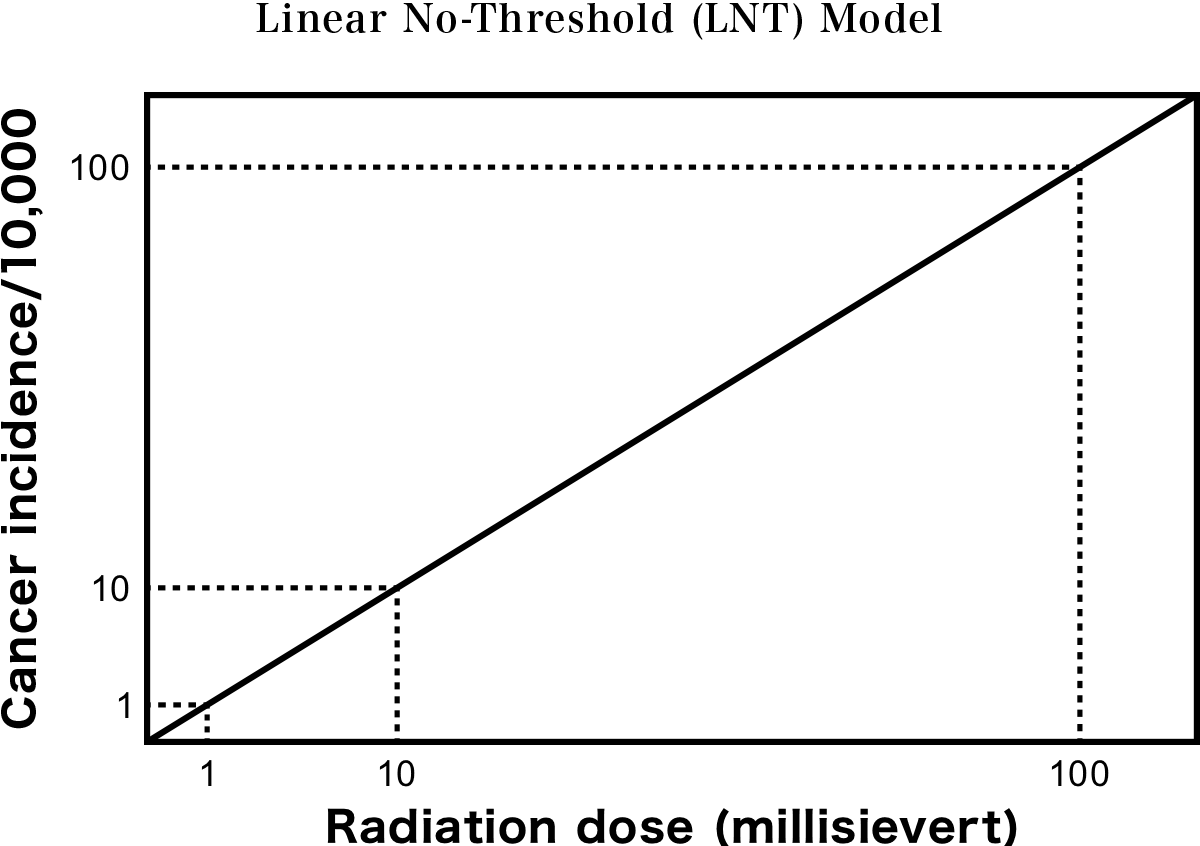
The ICRP has set the limit of public exposure to 1 millisievert per year and states that higher doses than 1 millisievert per year are unacceptable under normal circumstances. After the accident in Fukushima however, the Japanese government adopted the policy of allowing evacuees to return to their hometowns once the radiation levels fell to 20 millisieverts or below, claiming that this was a safe level of annual exposure.
Dose-dependent thyroid cancer induced by radiation exposure
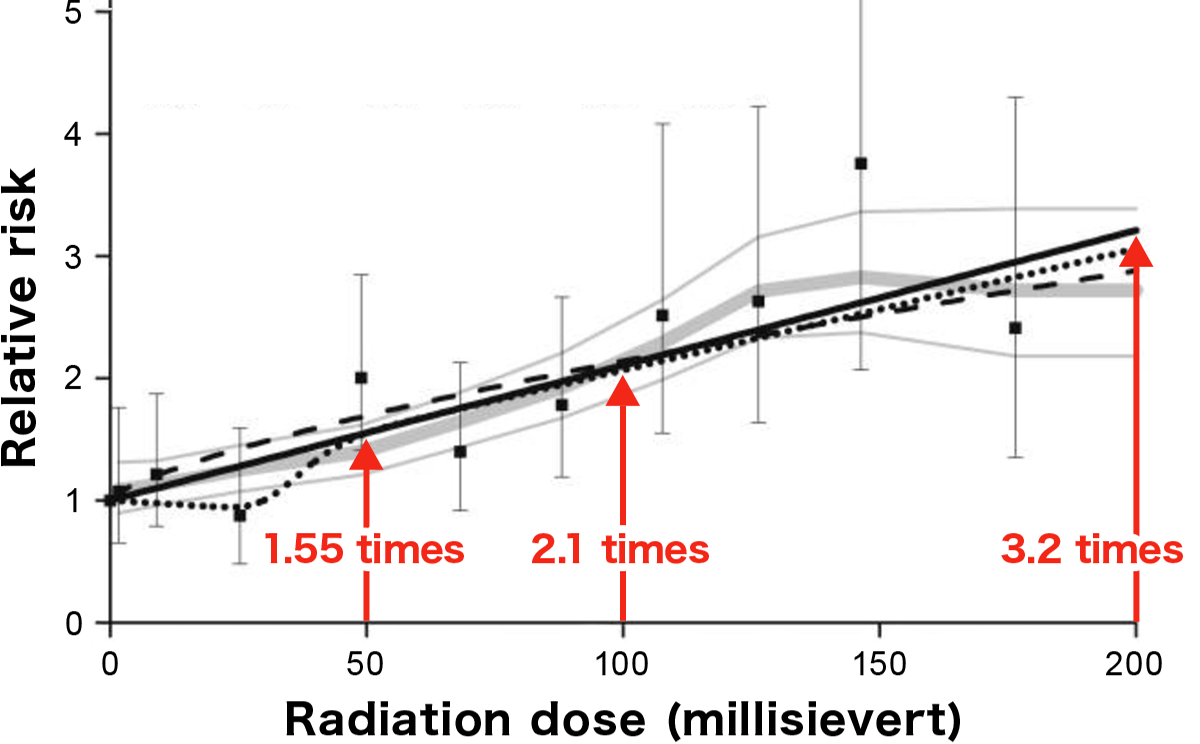
Thyroid cancer incidence among people who have actually been exposed to radiation is consistent with the Linear No-Threshold (LNT) model. Exposure of the thyroid gland to 50 millisieverts increases the incidence of thyroid cancer 1.55 times compared to those not exposed. The incidence of thyroid cancer increases linearly with increasing radiation dose.
2. What is 1 millisievert of radiation exposure?
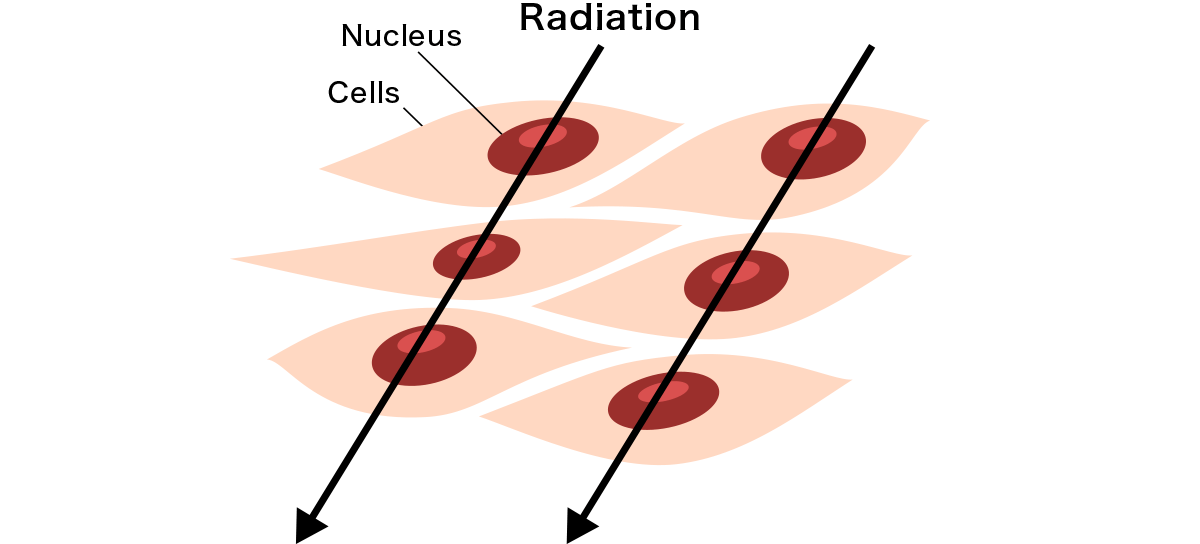
Exposure to 1 millisievert of radiation means that on average,1 ray of radiation passes through the nucleus of a cell. 5 millisieverts would mean 5 rays. The nucleus, located in the center of the cell, contains DNA, the blueprint of the body, which is a double-helix structure with two strands facing each other, as shown in the figure below. Protruding inward from the strand are the bases adenine (A), thymine (T), guanine (G), and cytosine (C), with A only forming a pair with T (A:T) and G with C (G:C). The order of these base pairs determines the type of protein that can be made. Radiation damages this DNA.
3. From radiation-induced DNA damage to carcinogenesis.
Since the energy of radiation is 15,000 to 20,000 times greater than the energy of the bonds between the atoms (chemical bonds) that make up DNA, the chemical bonds can be easily broken by radiation (direct action) and the surrounding base-pairs can be damaged. Depending on how the radiation hits the DNA, both strands may be broken (a double-strand break) or only one strand may be broken (a single-strand break). Even if radiation does not hit the DNA directly, it can damage the DNA indirectly by ionizing water in the cell, which produces harmful reactive oxygen species (indirect effects).
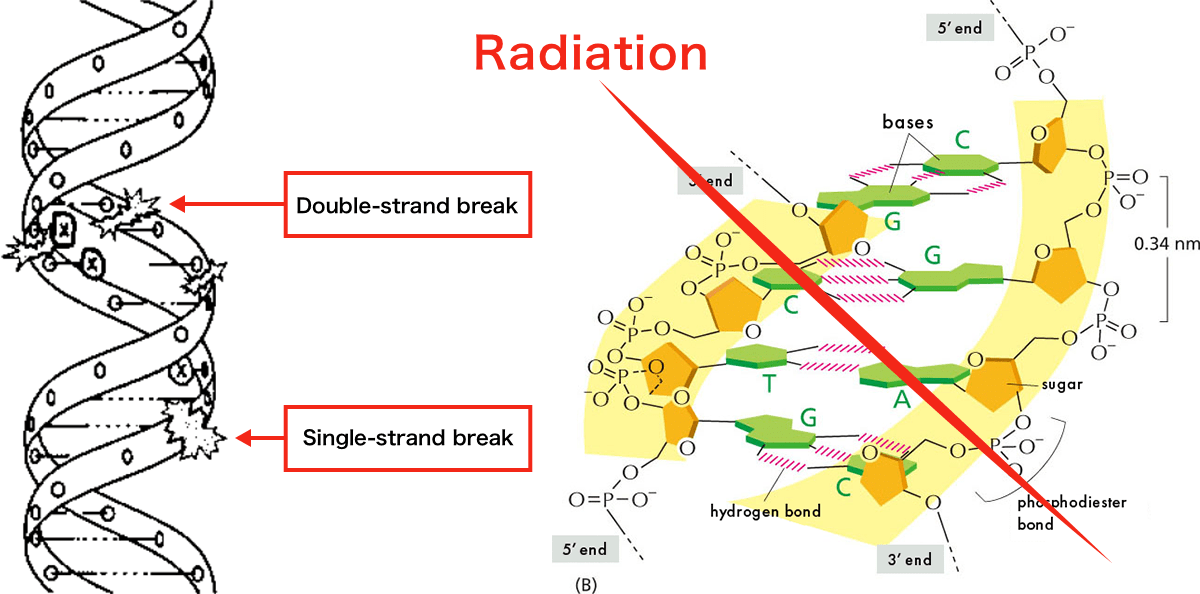
Source: Right; Alberts B. et al. [Molecular Biology of the Cell] (notations in read added by the 3.11 Fund)
Repair of single-strand breaks
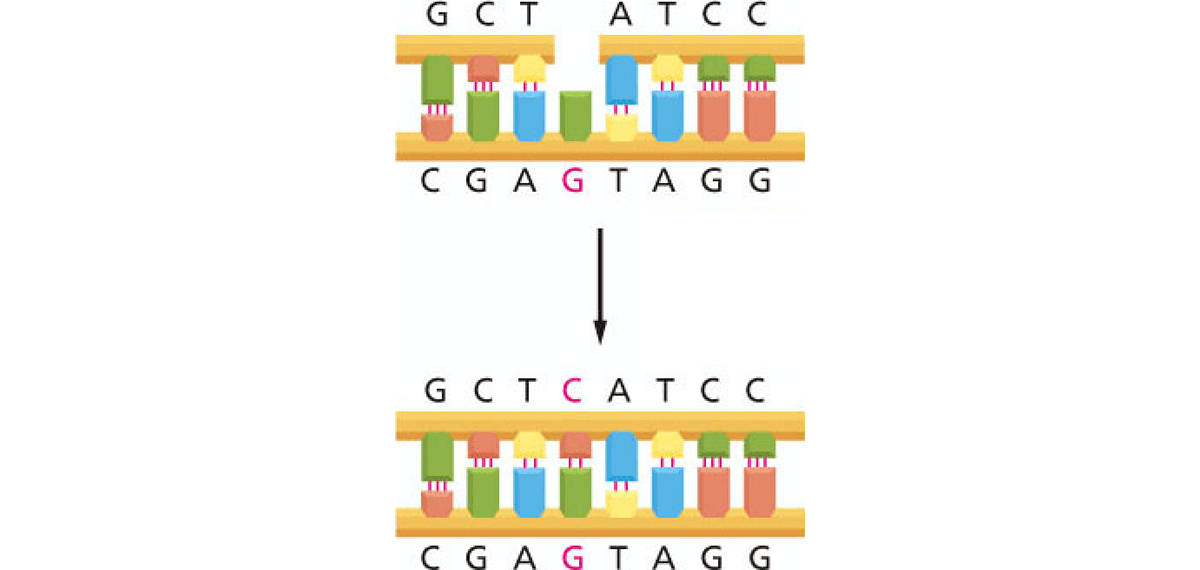
In the figure below, C is damaged by radiation and excised by enzymes. G is on the other strand of the DNA and is the only base that can be paired with C, so that spot will always be filled by C and the damage will be repaired correctly (as shown in the figure). DNA naturally gets damaged every day, but much of the time, the damage causes single strand breaks that can be repaired correctly.
The fate of double-strand breaks
In the case of double-strand breaks, however, base pairing cannot take place. The fate of such complex damage can be divided into three outcomes, as shown in the figure below.
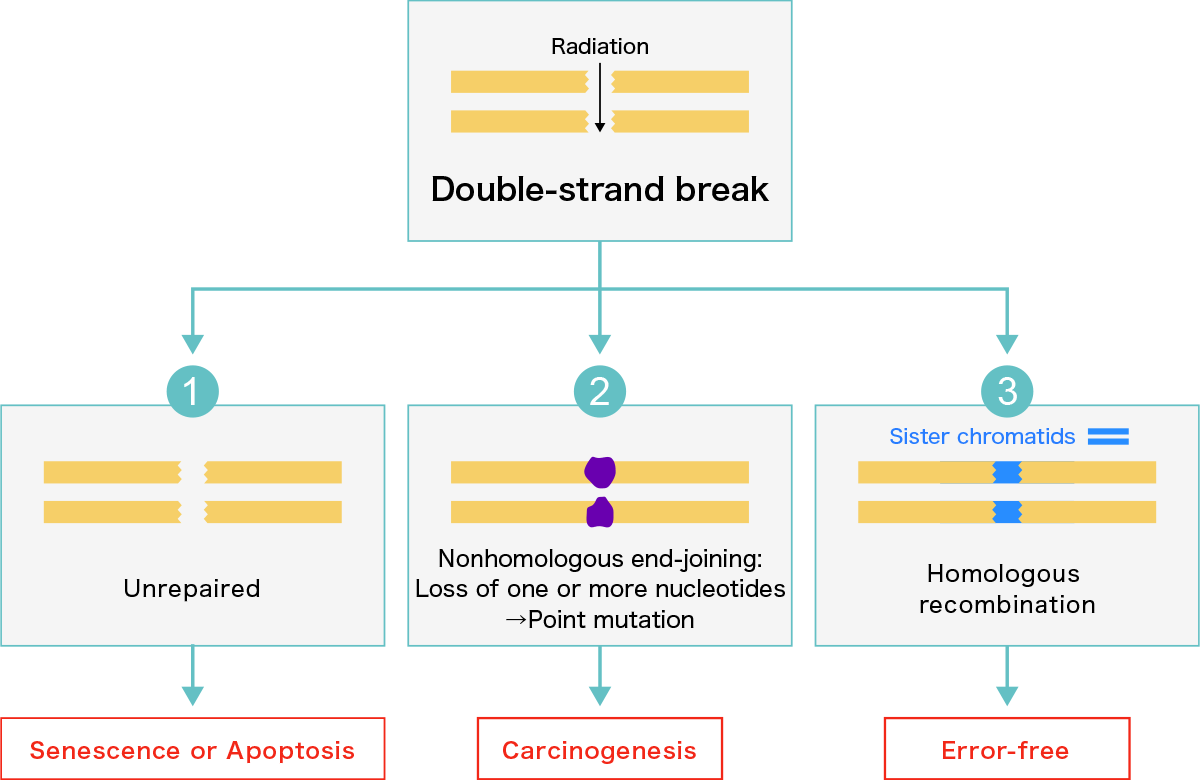
- If cells cannot repair the damage, they cannot divide, resulting in cell senescence (aging) or apoptosis (suicide of the cell). This is more likely to happen at high radiation doses, resulting in acute radiation syndrome, involving such manifestations as hair loss and purpura (internal bleeding).
- When two broken ends are incorrectly connected to each other, the intervening bases are lost, resulting in the alteration of the base sequence, leading to mutations, which can lead to carcinogenesis, the formation of cancer. (Nonhomologous end-joining).
- Sometimes error-free repairs occur. Each person receives a set of chromosomes from each parent. If one chromosome is damaged, a nearby intact sister chromatid DNA is used as a template to repair the damage correctly (Homologous recombination). The likelihood of this kind of error-free repair taking place is much less than that of a mutation occurring.
The fate of the cells depends on the exposure dose and the state of the cells at the time of exposure.
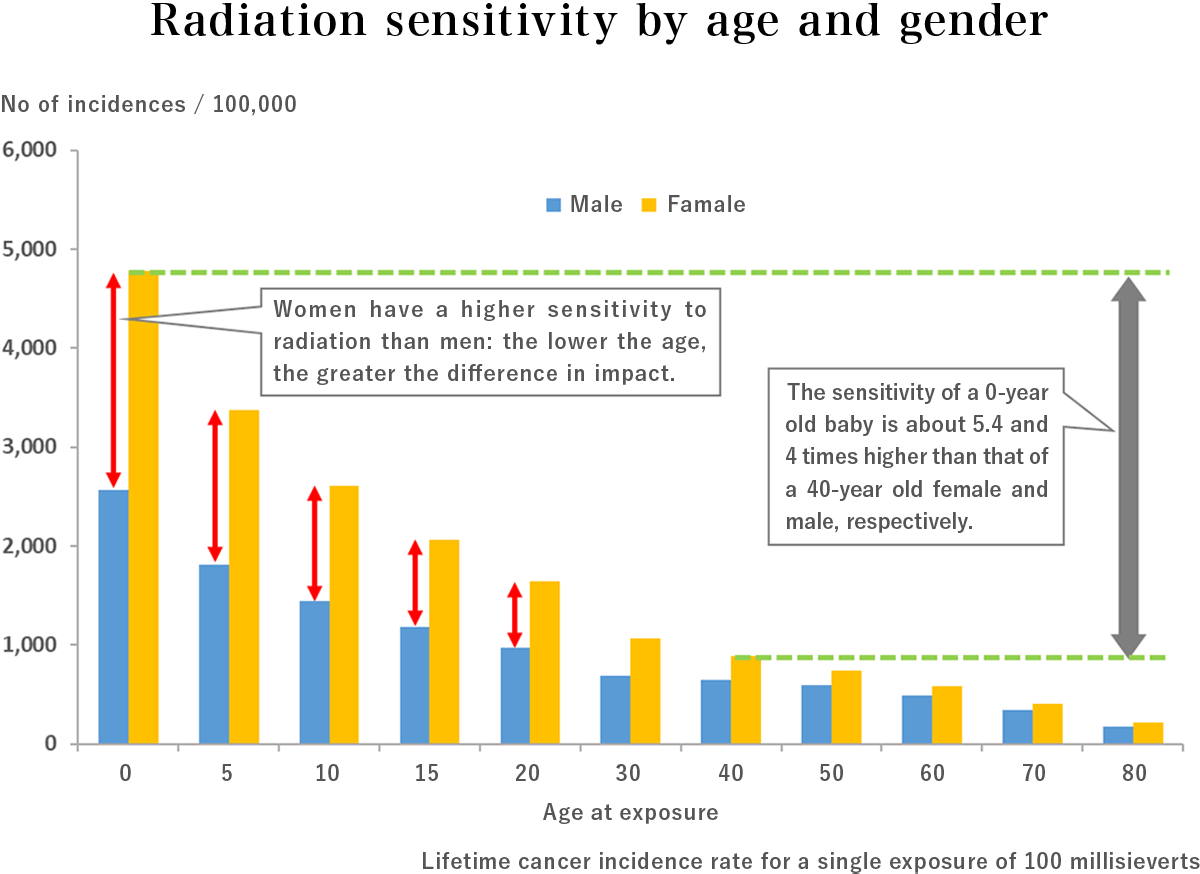
4. Fetuses and children are more vulnerable to radiation than adults.
Since the cells of fetuses and children are actively dividing, their DNA is more sensitive to radiation damage and thus they develop cancers more readily.
Fukushima Prefecture’s standard for evacuees to return to their homes is 20 millisieverts per year, which is actually the annual dose limit for radiation workers. When radiation workers are in radiation-controlled areas, they are not permitted to eat, drink or sleep, and those under 18 years old are not even allowed to enter. The 20 millisievert return policy contradicts such official workplace guidelines as it claims that it is safe for radiation sensitive individuals, pregnant women, infants and children, to go about their daily lives in such high-level radiation areas. Some citizens are currently suing the Japanese government in order to have this policy reversed.
Created: March 2021
-
Dose Dependency and the Mechanism of Carcinogenesis
-
The Nuclear Power Plant Accident and Thyroid Cancer
- Why did people worry about thyroid cancer after the Fukushima Nuclear Power Plant Accident?
- Why should people take iodine tablets (“stable iodine,” “potassium iodide”) in the event of a nuclear accident?
- When should iodine tablets be taken? What is the required dosage?
- Did the people of Fukushima Prefecture take iodine tablets?
-
Thyroid Examinations in Fukushima Prefecture after the TEPCO Nuclear Accident
- The thyroid examination system in Fukushima Prefecture.
- The high incidence of thyroid cancer in Fukushima Prefecture.
- Is there an association between the level of contamination and thyroid cancer incidence?
- An accurate thyroid cancer case count is essential.
- The decline in thyroid screening rate is a problem.
-
What Can We Do to Protect Children’s Health?

